At City Dermatology Clinic in London and Harley Street, our dermatologists and aesthetic doctors specialise in the safe, precise removal of sebaceous hyperplasia using medical-grade techniques that minimise scarring and protect surrounding skin. Your consultation is focused, straightforward, and fully tailored to your needs. We’ll confirm the diagnosis, rule out other conditions if necessary, and recommend the most effective treatment option for clear, smooth results.
Sebaceous hyperplasia can be safely and effectively treated using several dermatological techniques. The best method depends on the size, depth, and number of lesions, as well as your skin type and any history of scarring or sensitivity. After assessing your skin, the specialist will recommend the most appropriate option.
For deeper or persistent lesions, a minor surgical excision may be recommended. The dermatologist or plastic surgeon removes the enlarged gland through a tiny incision under local anaesthetic. This method ensures complete removal and is reserved for lesions that are atypical, unusually deep, or unresponsive to other treatments.
Electrocautery is one of the most effective treatments for sebaceous hyperplasia. A fine-tipped device applies controlled heat to the enlarged oil gland, flattening the lesion with precision. The procedure is quick, performed under local anaesthetic where required, and produces a small crust that heals over a few days. This method is often chosen for multiple lesions or areas where accuracy is essential.
Certain medical lasers can gently target the enlarged sebaceous glands, shrinking them without damaging surrounding skin. Laser treatment is particularly suitable for patients who prefer a non-contact approach or have clusters of facial lesions. Recovery is minimal, and redness typically settles within a short period.
In some cases, prescription-strength topical therapies such as retinoids may help reduce the appearance of mild sebaceous hyperplasia. These are not instant solutions and work best as adjuncts to in-clinic treatments or for preventing new lesions.
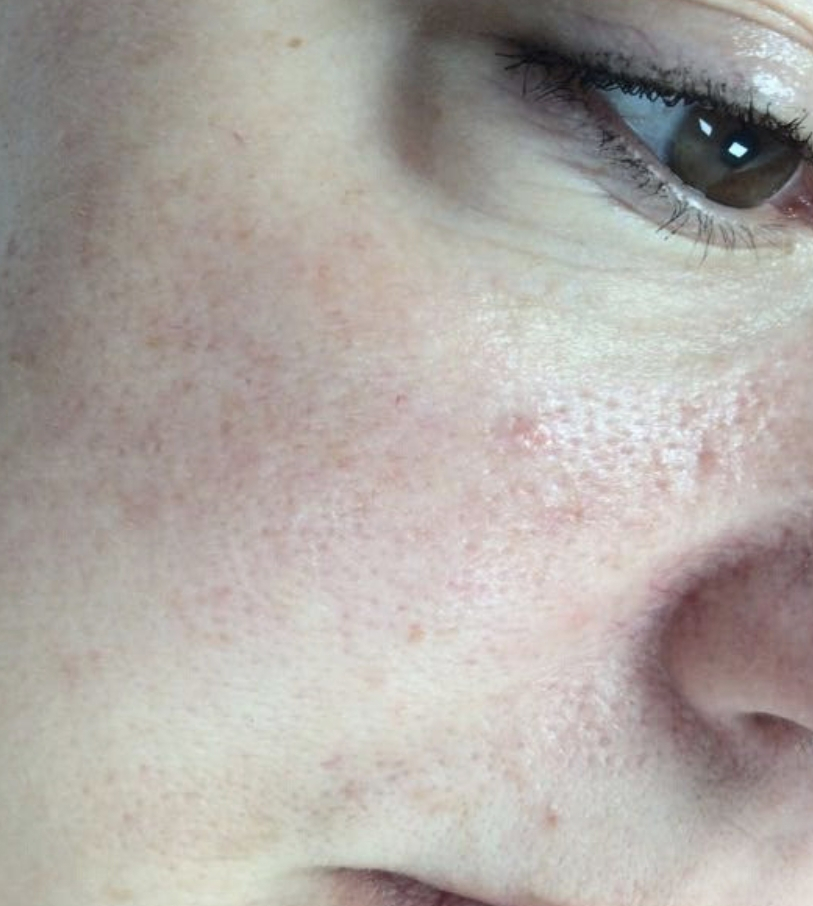
Sebaceous hyperplasia is a common, harmless skin condition where enlarged oil glands form small, soft bumps on the face, typically the forehead, cheeks, and nose. These bumps are usually flesh-coloured or yellowish with a shallow central dip, often mistaken for acne or basal cell carcinoma.
Although benign, many people seek removal when the bumps become more noticeable, increase in number, or affect cosmetic appearance. A proper diagnosis from a dermatologist or skin surgeon ensures the condition is correctly identified and any concerning lesions are ruled out before treatment.
Sebaceous hyperplasia is diagnosed through a clinical skin examination, often supported by dermoscopy to confirm the characteristic features, small, yellowish bumps with a central depression caused by enlarged oil glands. The condition is benign, but professional assessment ensures an accurate distinction from other facial lesions that may appear similar.
Removal becomes appropriate when lesions grow, become more visible, or cause cosmetic concern. Dermatologists also recommend assessment if the bumps change in colour, bleed, or fail to match the typical pattern of sebaceous hyperplasia, as these features may warrant further investigation. During your consultation, the doctor will confirm the diagnosis and outline the safest and most effective treatment options based on the number, location, and depth of the lesions.
Understanding what happens during and after sebaceous hyperplasia removal helps set clear expectations for comfort, recovery, and results. Procedures are carried out by dermatologists or aesthetic surgeons using precise, targeted methods that treat the enlarged gland while protecting surrounding skin.
| Stage | What to Expect |
|---|---|
| Initial Consultation | A dermatologist examines the lesion to confirm it is sebaceous hyperplasia and not a similar-looking condition. Dermoscopy is often used to assess depth and vascular patterns. Treatment options are discussed based on location, skin type, and the number of lesions. |
| Treatment Session | Performed using electrocautery, laser, or targeted cauterisation. The lesion is gently flattened by removing excess sebaceous tissue. Local anaesthetic may be used for comfort. Treatment usually takes 10–20 minutes depending on the number of areas treated. |
| Day 1–2 | Small crusts or pinpoint scabs form where the lesions were treated. Mild redness or sensitivity is normal. Keep the area clean and avoid makeup, exfoliants, or active skincare (retinol, acids). |
| Days 3–7 | Crusts begin to lift naturally. Redness gradually settles. Most people can resume normal skincare with gentle products. Sun protection is essential to prevent pigmentation changes. |
| Weeks 2–4 | New skin forms, creating a smoother surface. Any residual pinkness continues to fade. Makeup can usually cover the area completely. |
| Months 1–3 | Final results develop as skin texture normalises. If multiple lesions were treated, occasional maintenance sessions may be recommended. |
Sebaceous hyperplasia requires accurate diagnosis and careful removal, especially when the bumps appear on the face. At our London clinics, assessment and treatment are carried out by dermatologists and aesthetic surgeons with extensive experience in managing benign skin lesions. Each case is reviewed using dermoscopy to confirm the diagnosis, rule out anything that mimics sebaceous hyperplasia, and guide the safest treatment method.
Our specialists perform large numbers of sebaceous hyperplasia removals every year, using precise, minimally invasive techniques tailored to the size, depth, and location of each lesion. This includes advanced electrosurgery, targeted cautery, and surgical micro-excision where necessary. Treatment is designed to minimise recurrence, protect skin texture, and avoid unnecessary scarring, especially in cosmetically sensitive areas such as the forehead, cheeks, and nose.
Patients also receive clear aftercare guidance and follow-up if needed. This ensures the treated areas heal properly, redness settles as expected, and results blend naturally with the surrounding skin. For individuals with multiple lesions or persistent flare-ups, our clinicians also advise on longer-term skin management, including triggers, prevention strategies, and treatment options that may reduce future recurrence.
Our clinic is led by a team of consultant dermatologists and plastic surgeons with extensive experience in diagnosing and treating skin lesions, including sebaceous hyperplasia. Each doctor specialises in minor skin surgery, dermoscopy, and advanced removal techniques, ensuring safe, precise treatment for both cosmetic and medical cases. Patients are seen exclusively by trained specialists, with every procedure carried out in our regulated London clinics to maintain the highest clinical standards.
Our clinic is led by a team of consultant dermatologists and plastic surgeons with extensive experience in diagnosing and treating skin lesions, including sebaceous hyperplasia. Each doctor specialises in minor skin surgery, dermoscopy, and advanced removal techniques, ensuring safe, precise treatment for both cosmetic and medical cases. Patients are seen exclusively by trained specialists, with every procedure carried out in our regulated London clinics to maintain the highest clinical standards.

BSc, MBChB, FRCS

MD, PhD

MBBS, MRCS

MBBS, MD, MRCP

MB ChB FRCS

MBBS, MSc, FRCS

MBBS, MSc, FRCS

MA MBBS FRCS

MD, PhD, CCT

MD, MSc, FRCS, FEBOPRAS

BSc, MBChB, FRCS

MBBS, FRCS
Sebaceous hyperplasia is a benign enlargement of the oil glands, most commonly seen on the forehead, cheeks, and nose. The lesions appear as small, yellowish bumps with a central indentation. They are harmless but can increase in number over time, particularly in adults with oily skin or long-term sun exposure.
Sebaceous hyperplasia is not cancerous and does not turn into skin cancer. However, some skin cancers, particularly basal cell carcinoma, can resemble similar bumps. If a lesion looks atypical or behaves differently from your usual pattern, a dermatologist may recommend dermoscopic assessment or biopsy to rule out malignancy.
These bumps form when sebaceous glands become enlarged and clogged. Factors include genetics, oily skin, sun damage, hormonal changes, and natural ageing of the skin. The condition is not related to poor hygiene and is not contagious.
Removal is typically chosen for cosmetic reasons, especially when bumps become more noticeable, multiply, or affect confidence. Medical removal is recommended if a lesion changes rapidly, bleeds, becomes inflamed, or if there is any uncertainty about the diagnosis.
Common treatments include electrocautery, laser therapy, or minor surgical removal depending on the lesion type, depth, and location. Your dermatologist will recommend the safest and most effective option based on your skin type and the number of lesions present.
Treatment is usually comfortable. A small amount of local anaesthetic or numbing cream is used depending on the method. Patients typically feel mild warmth or pressure but no sharp pain.
Healing usually takes between 7–14 days, depending on the treatment method and the number of areas treated. Pinkness or mild crusting is normal and gradually fades. Most people return to everyday activities immediately.
Individual bumps do not regrow once properly treated, but new lesions can form over time if your skin is prone to them. Good sun protection and skincare may reduce recurrence.
Possible side effects include temporary redness, mild swelling, superficial scabbing, or pigmentation changes. Scarring is uncommon when treatment is performed by an experienced dermatologist.
Over-the-counter products and home remedies do not remove sebaceous hyperplasia. Squeezing or attempting to extract the bumps can cause scarring, bleeding, or infection. Safe removal should be carried out by a medical professional.
Most patients resume normal routines immediately. If electrocautery or laser is used, you may need to avoid heavy exercise, steam rooms, or direct sun for a short period to support healing.
A biopsy is not usually required. It is only recommended if the lesion appears atypical or if the dermatologist cannot confidently differentiate it from other conditions through dermoscopy.