Seborrheic keratosis and melanoma are frequently mentioned together because, in some cases, they can look similar to the untrained eye. Both may appear dark, uneven, raised, or irregular. Both can develop later in life. Both may prompt concern when they change in colour, size, or texture.
The confusion is not a patient failure. Even experienced clinicians approach pigmented lesions carefully, because visual similarity alone is not enough to make a safe judgement. This overlap is precisely why assessment is emphasised rather than reassurance based on appearance alone.
Understanding the general differences can help patients know when to seek review, but it does not replace clinical evaluation.
What is seborrheic keratosis?
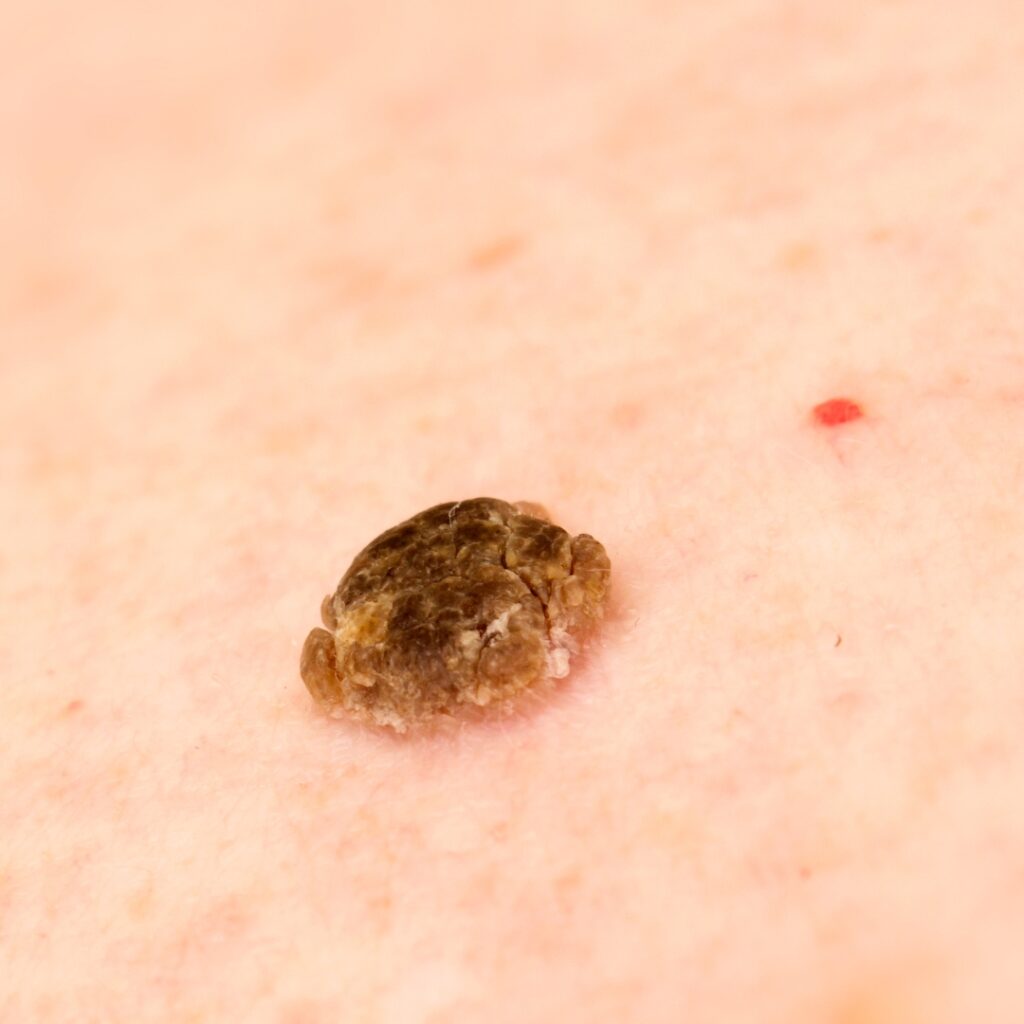
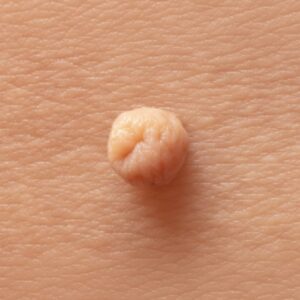
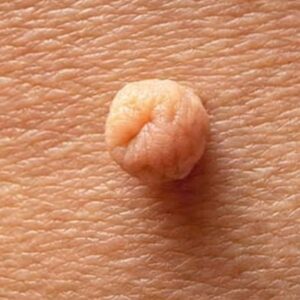
Seborrheic keratosis is a very common benign growth arising from the outer layer of the skin. It is not cancerous and does not turn into cancer. These lesions typically develop gradually and become more common with age.
Common features include:
- A waxy, scaly, or slightly rough surface
- A “stuck-on” appearance, as if the lesion is sitting on top of the skin
- Colour ranging from light tan to dark brown or black
- Well-defined edges, though shapes can vary
- A tendency to thicken slowly over time
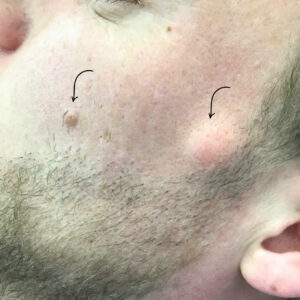
Seborrheic keratoses can appear almost anywhere on the body except the palms and soles. Many people develop multiple lesions over years. Some remain flat; others become raised or more textured.
Although harmless, seborrheic keratoses may itch, catch on clothing, or become inflamed. These changes can alter their appearance and increase anxiety, even though the underlying condition remains benign.
What is melanoma?
Melanoma is a malignant tumour of melanocytes, the pigment-producing cells of the skin. It is less common than benign lesions but requires prompt recognition because it can spread beyond the skin if untreated.
Melanoma does not have a single appearance. It may be:
- Dark brown or black
- Unevenly coloured
- Asymmetrical
- Flat or raised
- Pink, red, or even colourless in some cases
Some melanomas arise from existing moles; others develop as new lesions on previously normal skin. Change over time is often a key feature, but not all melanomas follow predictable patterns.
Because melanoma is variable, clinicians do not rely on one feature alone. Instead, they assess combinations of appearance, structure, history, and dermoscopic patterns.
Key visual differences clinicians look for
While no single sign is definitive, clinicians are trained to recognise patterns that favour one diagnosis over another.
Seborrheic keratosis often shows:
- A sharply demarcated border
- A surface that looks waxy, crumbly, or “pasted on”
- Uniform texture across the lesion
- Small surface features such as tiny pits or ridges
Melanoma may show:
- Asymmetry in shape or structure
- Irregular or poorly defined borders
- Variation in colour within the same lesion
- Areas that appear structureless rather than textured
Importantly, these features overlap. Some seborrheic keratoses are dark and irregular. Some melanomas can appear relatively uniform. This is why appearance alone is not sufficient for certainty.
Texture, surface change, and growth pattern
Texture is one of the reasons seborrheic keratosis is often mistaken for melanoma. As seborrheic keratoses thicken, they can become raised, crusted, or uneven. Inflammation or friction may cause redness or scabbing.
Clinicians consider:
- Whether the lesion feels superficial or integrated into the skin
- Whether the surface changes are uniform or patchy
- How quickly changes have occurred
Seborrheic keratoses usually evolve slowly over years. Melanoma may change more unpredictably, though this is not always rapid.
A sudden change in a long-standing lesion, or the appearance of a lesion that looks different from others on the body, often prompts closer examination regardless of suspected diagnosis.
The role of dermoscopy in assessment
Dermoscopy is a handheld examination technique that allows clinicians to see structures beneath the surface of the skin that are not visible to the naked eye.
Under dermoscopy:
- Seborrheic keratoses often show characteristic benign patterns, such as milia-like cysts or fissures
- Melanoma may show atypical pigment networks, irregular dots, streaks, or structureless areas
Dermoscopy does not provide a diagnosis in isolation, but it significantly improves diagnostic accuracy when used by trained clinicians. It is one of the key reasons why specialist assessment is recommended for uncertain or changing lesions.
When a lesion should be checked
Assessment is usually appropriate if a lesion:
- Is new and looks different from others on the body
- Has changed in size, shape, colour, or texture
- Bleeds, crusts, or becomes persistently inflamed
- Causes concern because it does not resemble existing benign lesions
This does not mean the lesion is dangerous. It means that uncertainty exists, and uncertainty is best resolved through examination rather than assumption.
Many benign lesions are assessed every day for reassurance alone. That reassurance is meaningful only when it is based on clinical evaluation.
Why self-diagnosis and photos are unreliable
Online images and comparison charts can be helpful for awareness, but they have limitations. Lighting, camera quality, angle, and skin type all affect how a lesion appears in photographs.
Two different lesions may look similar in a photo and very different under dermoscopy. Conversely, two lesions that look different online may share the same benign diagnosis.
Self-diagnosis often focuses on isolated features rather than overall pattern and context. Clinicians are trained to interpret combinations of signs, not individual characteristics in isolation.
What happens during a clinical assessment
A clinical assessment typically includes:
- Visual inspection of the lesion
- Dermoscopic examination
- Discussion of when the lesion appeared and how it has changed
- Consideration of the wider skin pattern, not just a single lesion
In some cases, no further action is required beyond reassurance. In others, monitoring, biopsy, or removal may be discussed. Decisions are based on clinical findings rather than patient anxiety alone, though patient concern is always taken seriously.
Assessment does not automatically lead to treatment. Its purpose is to clarify what the lesion is and whether any action is appropriate.