Many people seek mole mapping for reassurance. The idea of having every mole photographed and digitally tracked over time feels thorough, preventative, and safe – particularly in an environment where skin cancer awareness is high.
For patients with many moles, or those who feel uncertain about what is normal on their skin, mole mapping can sound like a logical solution. However, the value of mole mapping depends less on the technology itself and more on how it is used, who interprets it, and which patients it is applied to.
Mole mapping is not inherently good or bad. Its usefulness is conditional.
What mole mapping actually is
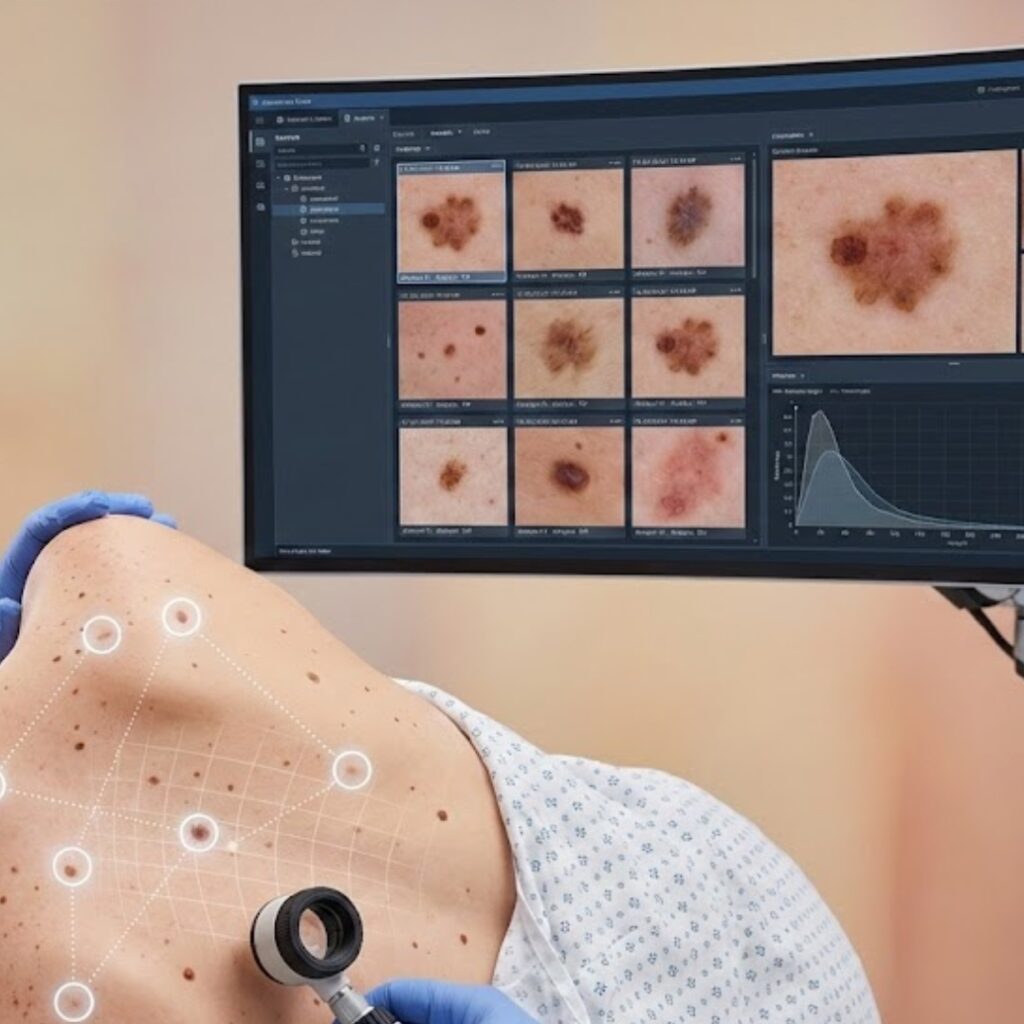
Mole mapping is a form of total-body photography, often combined with close-up images of selected moles. These images are stored and compared over time to identify visible change.
Some systems rely purely on photography. Others incorporate software or AI tools that highlight differences between visits. In all cases, mole mapping is a documentation and comparison tool, not a diagnostic test.
It records what the skin looks like. It does not determine whether a lesion is benign or malignant.
How mole mapping is performed
In practice, mole mapping usually involves:
- Standardised photographs of the body surface
- Close-up images of selected moles
- Repeat imaging at set intervals
- Visual or software-assisted comparison over time
In some clinics, images are taken by trained staff and later reviewed by a clinician. In others, photography is delegated to non-medical personnel, with remote review or automated flagging.
This distinction matters. Mole mapping is only as reliable as the clinical oversight behind it.
What mole mapping can be useful for
When used appropriately, mole mapping can provide genuine clinical value in selected patients.
Potential benefits include:
- Establishing a baseline in patients with a very high number of moles
- Helping identify new lesions that were not present previously
- Supporting long-term monitoring in patients with a personal history of melanoma
- Reducing unnecessary biopsies in carefully monitored high-risk individuals
In these contexts, mole mapping acts as a reference tool, not a shortcut to diagnosis.
The clinical limitations of mole mapping
Despite its appeal, mole mapping has important limitations that are often under-emphasised.
Key limitations include:
- It detects visible change, not malignancy
Some melanomas do not change noticeably in early stages. - It cannot assess subsurface structures
Photography shows the surface only. It cannot assess pigment networks or cellular patterns. - It can create false reassurance
A lesion that looks unchanged on photographs may still warrant concern on examination. - It may increase false alarms
Benign moles often change, especially in younger adults, leading to unnecessary anxiety or procedures.
Change alone is not a diagnosis. Stability alone is not a guarantee of safety.
Mole mapping vs dermatologist-led skin checks
A dermatologist-led skin check is an active clinical process, not a passive recording exercise.
It involves:
- Assessing individual lesions
- Evaluating the overall pattern of a patient’s moles
- Identifying lesions that stand out as different (the “ugly duckling” principle)
- Integrating personal and family history
Mole mapping does not perform these functions on its own. Without expert interpretation, it is incomplete.
In clinical practice, mole mapping is most valuable when it supports specialist assessment — not when it replaces it.
The role of dermoscopy
Dermoscopy is central to modern skin lesion assessment. It allows clinicians to visualise structures beneath the surface of the skin that cannot be seen with the naked eye or with standard photography.
Many early melanomas show dermoscopic features long before obvious surface change occurs. These features are not captured by mole mapping images.
For this reason, dermoscopy remains a more powerful diagnostic tool than photography alone.
Technology, AI, and questions of responsibility
Some mole mapping systems now incorporate AI-assisted analysis. While these tools may help highlight change, they do not remove the need for clinical judgement.
A critical question remains: who is responsible for the diagnosis?
- A camera does not diagnose.
- Software does not carry clinical accountability.
- Responsibility always rests with a qualified clinician.
Technology can assist, but it cannot replace trained interpretation or clinical decision-making.
Who may benefit most from mole mapping
Mole mapping may be considered for patients who:
- Have a very high number of moles
- Have a personal history of melanoma
- Have a strong family history of melanoma
- Are under structured, long-term dermatological follow-up
For people with only a few moles and no significant risk factors, routine mole mapping is unlikely to add meaningful clinical value beyond expert examination.
Common misconceptions
“Mole mapping finds melanoma early.”
It may help document change, but early detection still relies on clinical assessment and dermoscopy.
“If nothing changes, everything is fine.”
Some melanomas do not change visibly in early stages.
“It replaces a skin check.”
It does not. Mole mapping without examination is incomplete.
“More technology means more safety.”
More data does not automatically improve diagnostic accuracy.
What a thorough skin assessment involves
A comprehensive skin assessment typically includes:
- Full skin examination by a trained clinician
- Dermoscopic evaluation of individual lesions
- Consideration of personal and family risk factors
- Discussion of monitoring, biopsy, or removal where appropriate
Photography may be used selectively, but it is not the foundation of diagnosis.