Skin biopsy recovery varies depending on the type of biopsy performed, the location on the body, and individual healing factors. Most biopsy sites heal within two to four weeks, though complete tissue remodelling can take several months. Understanding what is normal during recovery helps patients manage expectations and identify signs that may require clinical review.
What Happens Immediately After the Biopsy
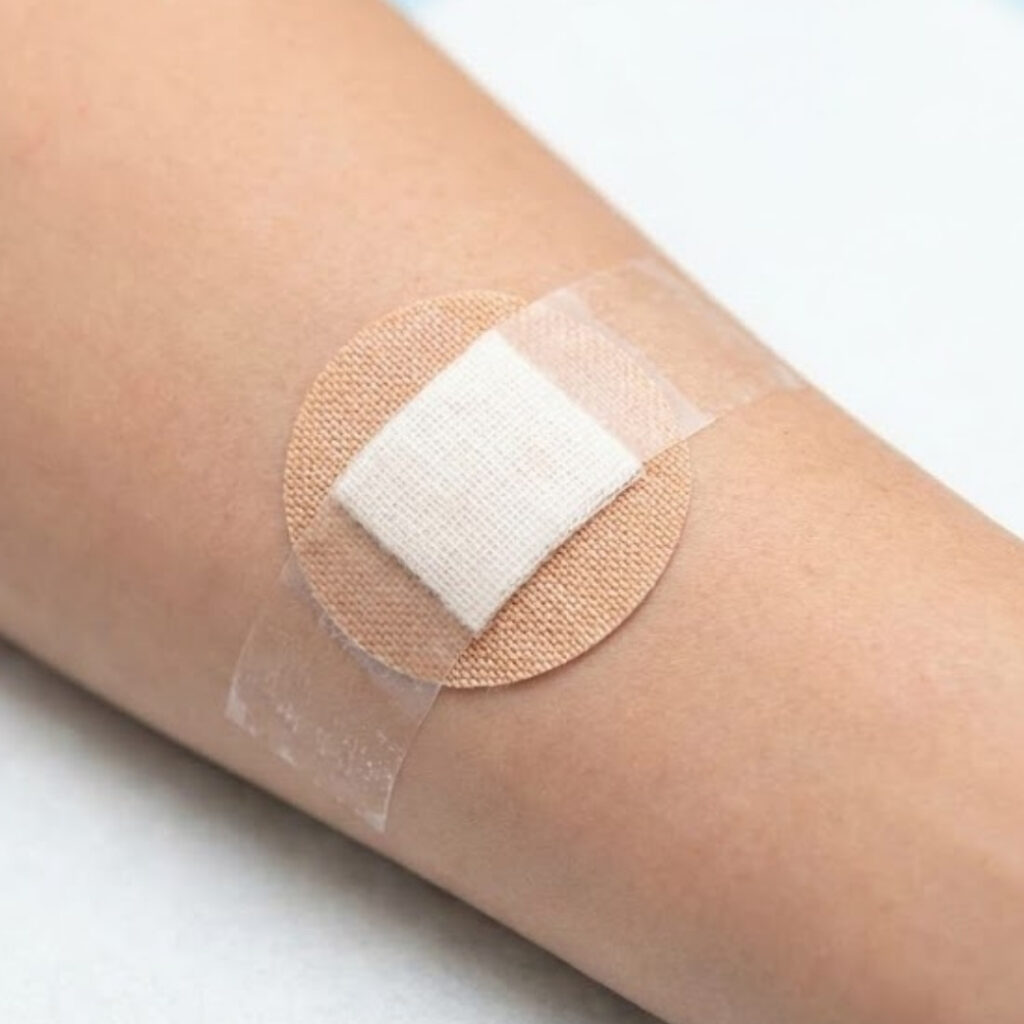
Once the biopsy is complete, the wound is dressed with a sterile dressing. Bleeding is controlled during the procedure using pressure, cautery, or topical agents, though minor oozing may occur in the first few hours.
The local anaesthetic typically wears off within 2-4 hours. Mild discomfort, throbbing, or a sensation of tightness around the wound is common as sensation returns.
Initial Wound Care
- Keep the dressing dry and intact for 24 hours unless instructed otherwise
- Avoid getting the wound wet during this period
- Rest the affected area where possible
- Elevate the site if it is on a limb to reduce swelling
- Take paracetamol if needed for discomfort (avoid aspirin or ibuprofen in the first 24 hours as these can increase bleeding risk)
What Is Normal in the First 24 Hours
- Mild aching or soreness around the biopsy site
- Small amount of blood spotting through the dressing
- Slight swelling or redness immediately around the wound
- Bruising beginning to appear, particularly on the face or areas with thin skin
What Is Not Normal
- Heavy bleeding that soaks through the dressing
- Severe pain that is not relieved by paracetamol
- Rapidly increasing swelling
- Fever or feeling unwell
If any of these occur, contact the clinic for advice.
Wound Care During the First Week
After 24 hours, the dressing can usually be changed. The wound may be left uncovered if it is dry and not in an area subject to friction or contamination. Some clinics recommend keeping the wound covered for several days, particularly if it is in a location prone to catching on clothing.
Daily care includes:
- Gently cleaning the wound with cooled boiled water or saline
- Patting dry with a clean towel or gauze
- Applying a thin layer of petroleum jelly or prescribed ointment if advised
- Covering with a fresh dressing if needed
Avoid soaking the wound in baths, swimming pools, or hot tubs during this phase. Showering is usually acceptable after 24-48 hours if the wound is patted dry afterwards.
What Healing Looks Like
During the first week, the wound edges begin to close. A scab or crust may form over the surface, which is part of the normal healing process and should not be picked or removed.
Normal appearances include:
- Redness around the wound edges
- Mild swelling
- Formation of a scab or crust
- Bruising that may spread slightly before fading
- Clear or slightly yellow fluid (serous discharge) in small amounts
The area may feel itchy as healing progresses. This is common and can be managed by keeping the skin moisturised around (but not directly over) the wound.
Activity and Movement
Light activity is usually acceptable, but avoid:
- Strenuous exercise or activities that cause sweating near the wound
- Heavy lifting if the biopsy is on the trunk or limbs
- Stretching or movements that pull on the wound edges
Facial biopsies generally tolerate normal activity better than those on the trunk or limbs, where movement and tension can delay healing.
Suture Removal Timing
If sutures were placed, they are typically removed between 7 and 14 days after the procedure, depending on the location:
| Body Area | Typical Suture Removal Time |
|---|---|
| Face | 5-7 days |
| Scalp | 7-10 days |
| Trunk | 10-14 days |
| Arms and legs | 10-14 days |
| Hands and feet | 10-14 days |
City Dermatology Clinic schedules suture removal appointments as part of routine aftercare. Approximately 35 suture removal appointments are conducted each month across both Harley Street and City of London locations.
Removing sutures too early can result in wound dehiscence (edges separating). Leaving them too long can increase scarring or allow suture marks to develop. The timing is determined based on the wound’s location and healing progress.
Suture Removal Process
Suture removal is quick and usually causes minimal discomfort. The wound edges should be well-approximated by this stage, though the scar will still be pink and slightly raised.
After suture removal, the wound no longer requires dressing in most cases, though it should be protected from sun exposure and trauma.
What Healing Looks Like at This Stage
By the end of the second week:
- The scab may have fallen off or be lifting at the edges
- The wound edges are closed
- Redness is beginning to fade but may still be noticeable
- The scar is forming and may appear slightly raised or firm
Itching can be more pronounced during this phase as collagen remodelling occurs beneath the surface.
The Maturation Phase
Once the wound has closed, the scar enters a maturation phase that lasts several months. During weeks 2-6, the scar gradually softens, flattens, and fades, though it will not reach its final appearance for 6-12 months.
What to expect:
- The scar remains pink or red for several weeks to months
- The texture may be slightly raised or firm initially
- Sensitivity around the scar is common
- Sun exposure can cause darkening (hyperpigmentation)

Ongoing Care
During this phase:
- Keep the scar moisturised with a simple emollient
- Apply broad-spectrum SPF 30+ sunscreen to the scar when exposed to sunlight
- Avoid picking or scratching the scar
- Massage the scar gently after 3-4 weeks if advised by your clinician
Some patients use silicone gel or sheets to support scar maturation, though evidence for their effectiveness varies. Discuss this with your clinician if you have concerns about scarring.
Recovery by Biopsy Type
Punch Biopsy Recovery
Typical healing time: 2-4 weeks
Punch biopsies create small, circular wounds. If sutured, healing is usually straightforward. If left to heal by secondary intention (without sutures), the wound takes longer to close but may result in a less visible scar.
Recovery characteristics:
- Minimal discomfort after the first few days
- Scab formation common if not sutured
- Final scar is usually a small, round mark 2-4mm in diameter
- Scarring is generally less noticeable on the face than on the trunk
Shave Biopsy Recovery
Typical healing time: 1-3 weeks
Shave biopsies remove only the superficial layers of skin and are not sutured. They heal by re-epithelialisation, where skin cells grow across the wound from the edges.
Recovery characteristics:
- Less discomfort than sutured biopsies
- Wound may weep clear fluid for several days
- Scab formation is common
- Final scar is usually flat or slightly depressed
- Often less noticeable than sutured scars, particularly on the face
Excisional Biopsy Recovery
Typical healing time: 2-6 weeks
Excisional biopsies involve full-thickness removal of a lesion and surrounding margin, with wound closure using sutures. These create linear scars and require more involved aftercare.
Recovery characteristics:
- More discomfort in the first few days due to deeper tissue involvement
- Sutures remain in place for 7-14 days depending on location
- Activity restrictions are more significant
- Final scar is linear and length depends on the size of the lesion removed
- Scarring is more variable and depends heavily on location and tension
At City Dermatology Clinic, excisional biopsies are performed by consultant plastic surgeons including Mr Parviz Sadigh, Mr Reza Alamouti, and Dr Jana Torres-Grau, who use techniques to minimise tension and optimise cosmetic outcomes where possible.
Scarring (What to Expect)
Scar Formation Is Normal
All skin biopsies result in a scar. The size, colour, and texture of the scar depend on multiple factors including biopsy type, location, technique, and individual healing response.
General scar characteristics:
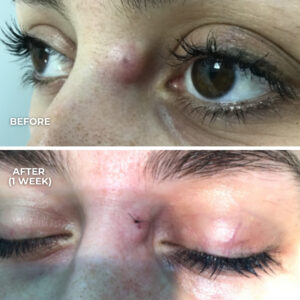
- Initial redness that fades over 6-12 months
- Slight firmness or elevation in the early months
- Gradual flattening and softening
- Final scar colour often slightly lighter or darker than surrounding skin
Factors That Influence Scarring
Location:
- Facial scars often heal well due to good blood supply
- Chest, shoulders, and back are prone to wider or more raised scars
- Scars over joints may stretch due to movement
Skin type:
- Individuals with darker skin may develop hyperpigmentation (darkening) or keloid scars
- Fair skin may show more redness initially but often fades well over time
Technique:
- Sutured wounds generally result in finer scars than wounds left to heal by secondary intention
- Tension on the wound edges increases scar width
Individual factors:
- Age, genetics, and overall health all influence healing
- Some individuals form thicker or more noticeable scars regardless of technique
Abnormal Scarring
Hypertrophic scars: Raised, thick scars that remain within the boundary of the original wound. These can develop in areas of high tension and may improve with time or treatment.
Keloid scars: Scars that grow beyond the original wound boundary and can be itchy or uncomfortable. Keloid formation is more common in certain skin types and body locations (chest, shoulders, earlobes).
If abnormal scarring develops, treatment options such as steroid injections, silicone therapy, or laser treatment may be discussed during follow-up. City Dermatology Clinic conducts approximately 7 keloid and scar treatment consultations each month.
Realistic Expectations
Scars are permanent. While they fade and soften over time, they do not disappear. The goal of good biopsy technique and aftercare is to minimise scarring, not eliminate it.
Patients concerned about scarring should discuss this during the initial consultation, as biopsy site selection and technique can sometimes be adjusted to reduce cosmetic impact where clinically appropriate.
Activity Restrictions and Wound Care
First Week Restrictions
- Avoid vigorous exercise, heavy lifting, or activities that cause sweating
- Do not submerge the wound in water (baths, swimming, hot tubs)
- Avoid alcohol in the first 24-48 hours as it can increase bleeding risk
- Refrain from smoking, which impairs healing
Weeks 2-4 Restrictions
- Gradual return to normal activity once sutures are removed and the wound is closed
- Avoid high-impact activities or contact sports until the scar has matured
- Protect the scar from sun exposure
Long-Term Care
- Apply sunscreen to the scar for at least 6-12 months to prevent hyperpigmentation
- Moisturise regularly to support scar softening
- Avoid trauma to the area
Signs of Normal Healing vs Complications
Normal Healing Signs
- Mild redness and swelling that gradually improves
- Clear or slightly yellow discharge in small amounts
- Scab formation
- Itching as healing progresses
- Bruising that fades over 1-2 weeks
Signs That Require Clinical Review
Infection:
- Increasing pain, redness, or swelling after the first few days
- Pus or foul-smelling discharge
- Warmth around the wound
- Fever or feeling unwell
Wound dehiscence (edges separating):
- Gap appearing between wound edges
- Bleeding from a previously closed wound
Allergic reaction:
- Rash or blistering around the wound
- Severe itching
Delayed healing:
- Wound not showing signs of closure after 2 weeks
- Persistent discharge or non-healing scab
City Dermatology Clinic conducts over 40 wound check appointments each month as part of routine aftercare. Patients can attend either Harley Street or City of London locations for follow-up if concerns arise.
Most complications are treatable if identified early. Do not wait if something does not seem right.
Factors That Influence Healing
Age
Younger patients generally heal faster and with less noticeable scarring, though this is not absolute. Older skin may take longer to heal and scars may be wider, though older patients often experience less inflammation.
Medical Conditions
Conditions that impair healing include:
- Diabetes
- Autoimmune diseases
- Poor circulation
- Immunosuppression (e.g., due to medication or illness)
Patients with these conditions should inform their clinician before the biopsy so that appropriate aftercare can be planned.
Medications
Certain medications affect healing:
- Anticoagulants (blood thinners) increase bleeding risk
- Corticosteroids delay wound closure
- Immunosuppressive drugs increase infection risk
Do not stop prescribed medications without consulting your prescribing doctor, but inform the biopsy clinic of all medications you take.
Smoking
Smoking reduces blood flow to healing tissues and significantly delays recovery. Smokers are advised to stop or reduce smoking for at least two weeks before and after the procedure.
Nutrition
Adequate protein, vitamin C, and zinc support healing. Poor nutrition can delay recovery, particularly in patients with restrictive diets or underlying health conditions.