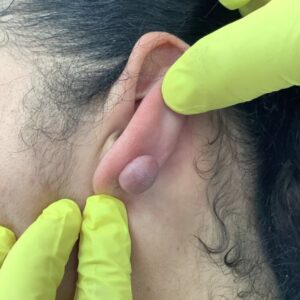
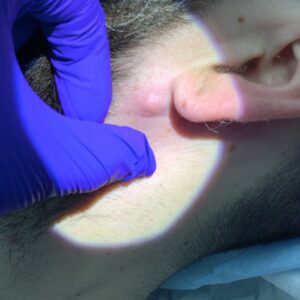
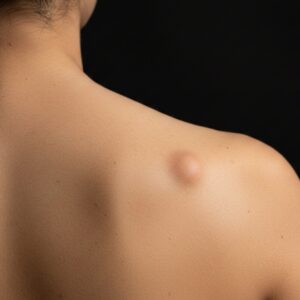
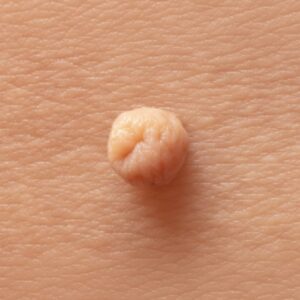
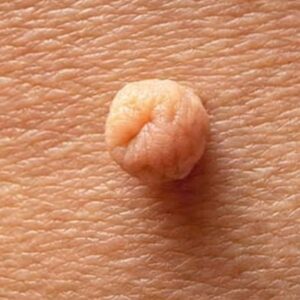
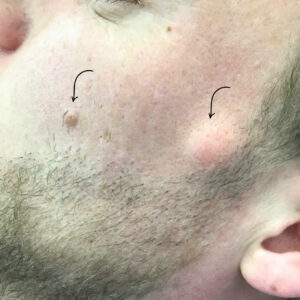
Epidermal naevi are non-cancerous skin growths that develop from the outermost layer of skin (the epidermis). They are usually present from birth or appear during early childhood, and may vary in size, colour, and texture. While epidermal naevi are benign, many people seek assessment to understand the nature of the lesion, address cosmetic concerns, or discuss removal options. Suitability for treatment depends on factors including lesion type, location, size, and individual circumstances, which are assessed during a dermatology consultation.
Assessment & Treatment Options
The choice of technique depends on lesion type, depth, location, cosmetic goals, and clinical assessment. Not all epidermal naevi are suitable for removal, and some may be better managed through observation.
Assessment Process
Assessment begins with a dermatology consultation, during which a clinician examines the lesion to confirm its type and characteristics. Epidermal naevi can vary significantly in appearance, and some may resemble other skin conditions. Dermoscopy (a magnified examination of the skin) may be used to assess features in detail. In some cases, a biopsy may be recommended to confirm the diagnosis, particularly if the lesion has changed or if uncertainty exists.
Treatment Approaches
Treatment is not always necessary, and some epidermal naevi may be managed conservatively with observation. When removal is appropriate, the following options may be considered:
Surgical Excision
Complete removal of the lesion and surrounding tissue. This approach aims to remove the full depth of the naevus, though recurrence is possible if some cells remain. Scarring will occur, and the appearance depends on lesion size, location, and individual healing.
Shave Removal
Removal of the raised portion of the lesion, typically used for superficial epidermal naevi. This method may not remove deeper skin layers, and recurrence is more likely than with full excision.
Laser Therapy
Used in some cases to reduce the appearance of certain types of epidermal naevus. Effectiveness varies depending on lesion characteristics, and multiple sessions may be required.
Conservative Management
Observation may be appropriate for small, asymptomatic lesions, particularly in children, where treatment can be deferred until later if desired.
Types of Epidermal Naevus
Epidermal naevi are classified based on their appearance and distribution:
Linear Epidermal Naevus
The most common type, appearing as a line or streak of thickened, warty skin. These often follow patterns known as Blaschko’s lines, which reflect developmental pathways in the skin. Linear epidermal naevi may appear on the limbs, trunk, or face.
Systematic Epidermal Naevus
More extensive lesions covering larger areas of skin. These may be associated with other developmental differences, though many occur in isolation without other concerns.
Inflammatory Linear Verrucous Epidermal Naevus (ILVEN)
A variant that may appear inflamed, red, or itchy. These lesions can cause discomfort and are sometimes more challenging to treat.
Naevus Sebaceus
A type of epidermal naevus that affects sebaceous (oil-producing) glands, typically appearing on the scalp or face as a hairless, waxy patch. These may change at puberty due to hormonal influences.
Keratinocytic Epidermal Naevus
Composed primarily of keratinocytes (the main skin cells). These lesions are typically raised, rough, or warty in texture and can vary in colour from skin-toned to brown.
Why People Seek Assessment or Removal
Reasons for seeking specialist review of an epidermal naevus include:
Cosmetic Concerns
Epidermal naevi on visible areas such as the face, neck, or arms may cause self-consciousness. Some lesions are raised, textured, or discoloured, which can affect how individuals feel about their appearance.
Changes in the Lesion
While epidermal naevi are benign, changes in size, colour, texture, or symptoms such as bleeding or discomfort may prompt assessment to rule out other conditions or complications.
Irritation or Discomfort
Lesions in areas subject to friction (such as the waistband, neckline, or underarms) may become irritated by clothing or movement. Some epidermal naevi can become inflamed or itchy.
Uncertainty About Lesion Type
Parents of children with congenital lesions, or adults who notice a lesion for the first time, may seek assessment to understand what it is and whether it requires treatment or monitoring.
Reassurance
While epidermal naevi are not cancerous, individuals may wish to confirm the diagnosis and receive guidance on whether observation or removal is more appropriate.
Risks Associated with Removal
Any procedure that removes skin tissue carries risks, which vary depending on the method used:
- Scarring: All removal methods will leave a scar. The size and appearance depend on lesion size, location, removal technique, and individual healing. Facial and visible area scars may be more noticeable.
- Recurrence: Epidermal naevi can recur if cells remain after removal, particularly with shave techniques or superficial methods. Full excision reduces recurrence risk but does not eliminate it entirely.
- Infection: As with any procedure, there is a risk of infection, though this is uncommon with appropriate wound care.
- Pigmentation changes: The treated area may heal lighter or darker than surrounding skin, particularly in individuals with darker skin tones.
- Incomplete removal: Complex or deep lesions may not be fully removable in a single procedure.
Recovery and Healing
Recovery time varies depending on the procedure and lesion location:
- Surgical excision: Healing typically takes 2-4 weeks. Sutures may be required and are usually removed within 7-14 days. Scarring evolves over several months.
- Shave removal: Surface healing occurs within 1-2 weeks, though pigmentation changes may take longer to settle.
- Laser therapy: Redness and swelling are common for several days following treatment. Multiple sessions may be spaced weeks apart.
Wound care instructions will be provided following any procedure. Individual healing varies, and factors such as age, skin type, lesion location, and general health influence recovery.
Suitability Considerations
Not all epidermal naevi are suitable for removal. Assessment considers:
- Lesion size and location: Large or complex lesions may require staged removal or may not be fully removable. Lesions in cosmetically sensitive areas (such as the face) require careful planning.
- Patient age: Treatment in young children is sometimes deferred unless the lesion causes functional problems or significant distress.
- Skin type and scarring risk: Individuals prone to keloid scarring or hyperpigmentation may not be suitable candidates for certain removal methods.
- Lesion characteristics: Deeply rooted or extensive lesions may have limited treatment options.
A dermatology consultation assesses individual suitability and discusses realistic expectations for outcomes. Not all patients will be suitable candidates for removal, and conservative management may be advised in some cases.