Human papillomavirus, commonly known as HPV, is one of the most prevalent viral infections worldwide. It affects the skin and mucous membranes, with over 100 different strains identified. While many people associate HPV exclusively with cervical cancer, most strains cause far less serious conditions, including common warts, verrucas, and genital warts.
Understanding HPV is important because the virus is extremely common. Most sexually active people will contract at least one strain of HPV during their lifetime, often without knowing it. This article explains what HPV is, how it spreads, which symptoms to watch for, and what treatment options are available at our central London clinic.
What Is Human Papillomavirus?
HPV is a group of more than 100 related viruses. Each HPV type is assigned a number, which helps doctors and researchers identify which strain is present. The virus infects the top layer of skin and can remain dormant for months or years before any visible symptoms appear.
HPV types are generally categorised into two groups: low-risk and high-risk. Low-risk strains, such as HPV 6 and HPV 11, typically cause benign growths like common warts and genital warts. High-risk strains, including HPV 16 and HPV 18, are associated with certain cancers, particularly cervical cancer, though cancer development is rare and usually takes many years.
The body’s immune system clears most HPV infections naturally within two years. However, some strains persist, leading to ongoing symptoms or complications. This is why monitoring and, in some cases, treatment become necessary.
How HPV Spreads
HPV spreads through direct skin-to-skin contact. This includes both sexual and non-sexual transmission. Genital HPV is primarily transmitted through vaginal, anal, or oral sex, even when the infected person has no visible symptoms. Condoms reduce the risk of transmission but do not eliminate it entirely, as HPV can infect areas not covered by a condom.
Non-genital HPV strains that cause common warts and verrucas spread through touch or contact with contaminated surfaces. Children often contract these types in schools, swimming pools, or communal changing areas. Minor cuts or abrasions in the skin make transmission easier, as the virus enters through broken skin barriers.
You cannot contract HPV from toilet seats, swimming pools, or sharing towels alone. However, walking barefoot in damp communal areas can increase your risk of plantar warts, caused by specific HPV types.
It is worth noting that HPV can be transmitted even when warts or other visible symptoms are not present. Many people carry the virus without knowing, which contributes to its widespread nature.
Symptoms and Types of HPV Infection
Most HPV infections cause no symptoms at all. The virus remains in the body silently and is eventually cleared by the immune system. When symptoms do occur, they vary depending on the type of HPV involved.
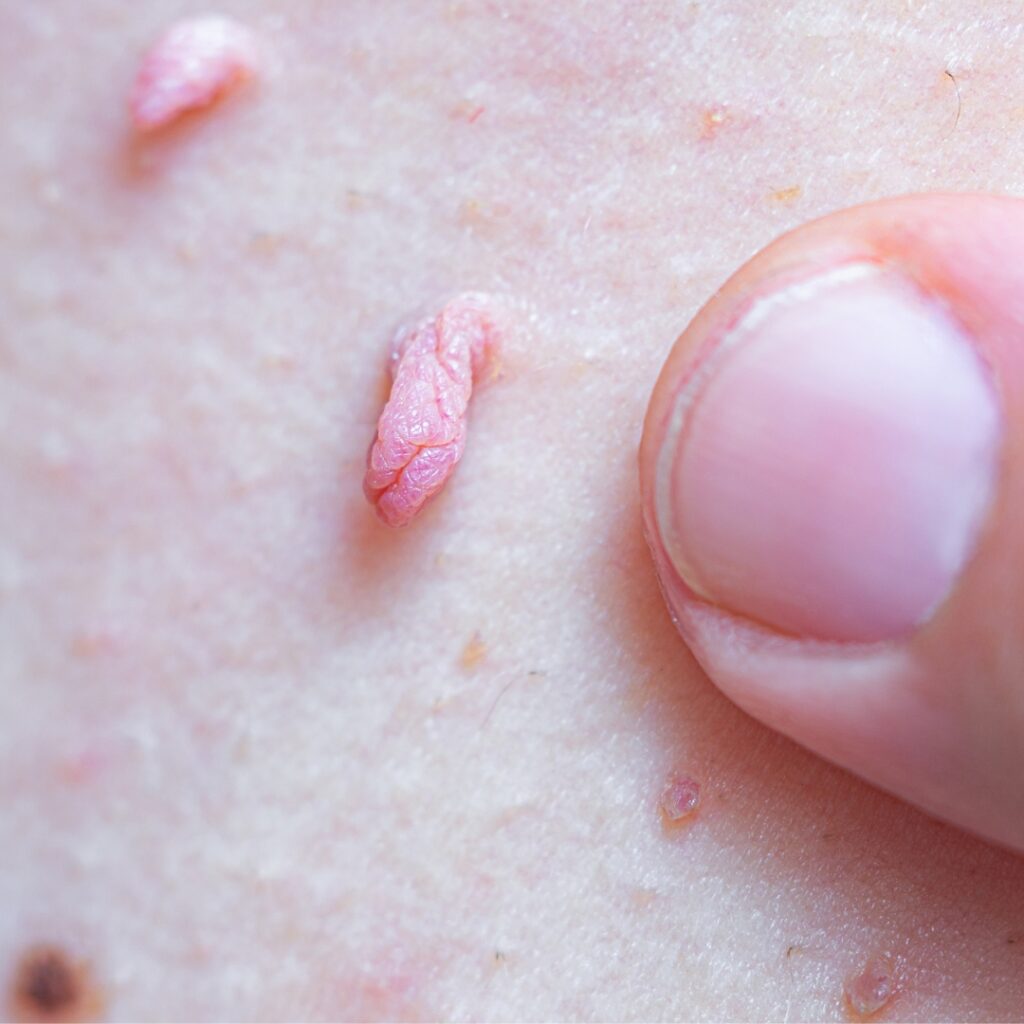
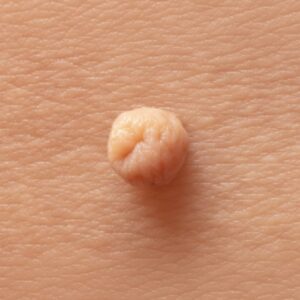
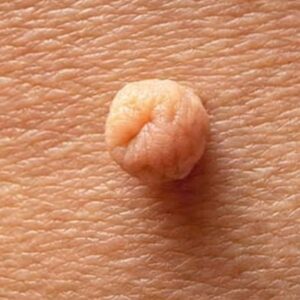
Common warts appear as rough, raised bumps on the hands, fingers, or around the nails. These are usually caused by HPV types 2, 4, or 7. They are harmless but can be unsightly or catch on clothing, prompting removal.
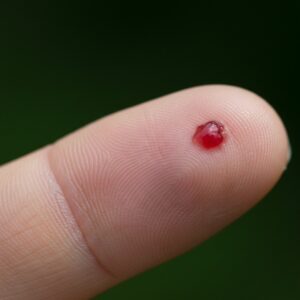
Plantar warts, or verrucas, develop on the soles of the feet. They grow inward due to pressure from walking and can be painful. Black dots often appear in the centre, which are small blood vessels. Plantar warts are caused by HPV types 1, 2, or 4.
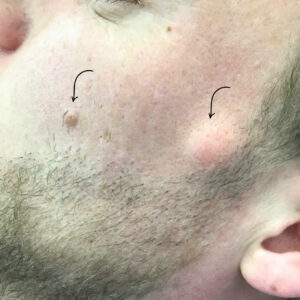
Flat warts are smaller and smoother than common warts. They often appear in clusters on the face, neck, or legs, particularly in children and young adults. These are typically caused by HPV types 3, 10, or 28.
Genital warts are soft, flesh-coloured growths that appear around the genital or anal area. They can be flat or cauliflower-shaped and may cause itching or discomfort. Most genital warts are caused by HPV types 6 and 11. Though not dangerous, they can cause distress and should be assessed by a specialist.
In rare cases, high-risk HPV strains cause changes in cells that may lead to cancer over many years. These strains usually do not cause visible symptoms, which is why routine cervical screening is important for early detection.
Diagnosing HPV
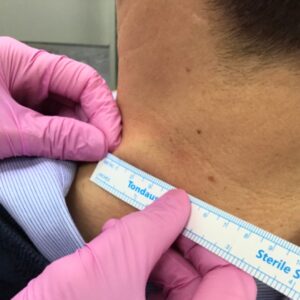
Most non-genital warts are diagnosed through visual examination. A dermatologist or experienced doctor can usually identify the type of wart by its appearance and location. No laboratory tests are needed in straightforward cases.
Genital warts are also diagnosed visually during a clinical examination. In some cases, a biopsy may be recommended if the diagnosis is uncertain or if the growth looks unusual. This involves taking a small sample of tissue for laboratory analysis.
For high-risk HPV strains associated with cervical changes, HPV testing is done as part of cervical screening programmes. Women aged 25 to 64 in the UK are invited for regular smear tests, which detect abnormal cervical cells before they become cancerous. HPV testing is now integrated into this process.
At City Dermatology Clinic, consultations for warts and skin growths are available on the same day. Our consultant dermatologists and plastic surgeons assess your condition in person, provide an accurate diagnosis, and discuss appropriate treatment options immediately.
Treatment Options for HPV-Related Warts
There is no cure for the HPV virus itself. However, the visible symptoms such as warts can be effectively treated. Treatment does not eliminate the virus from your body, but it removes the growths and reduces transmission risk.
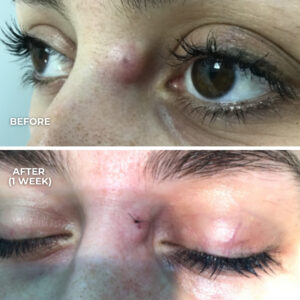
Cryotherapy involves freezing the wart with liquid nitrogen. The extreme cold destroys the tissue, causing the wart to fall off within one to two weeks. Multiple sessions may be needed for stubborn warts. Cryotherapy is quick and effective, though it can cause temporary discomfort.
Electrosurgery uses a heated probe to burn away the wart tissue. This method is particularly useful for larger or more resistant warts. The procedure is performed under local anaesthetic, making it painless. Healing usually takes one to two weeks, with minimal scarring.
Surgical excision involves cutting out the wart under local anaesthetic. This is often used for deeper warts, such as plantar warts, or when other treatments have failed. The wound is closed with stitches if necessary, and recovery is typically straightforward.
Topical treatments, including salicylic acid or prescription creams, can be applied at home over several weeks. These work by gradually dissolving the wart tissue. They are less invasive but require patience and consistent application.
For genital warts, topical treatments such as podophyllotoxin or imiquimod are commonly prescribed. These are applied by the patient at home following specific instructions. Alternatively, cryotherapy or surgical removal can be performed in clinic.
At City Dermatology Clinic, we offer same-day wart removal for most patients. Our plastic surgeons and dermatologists use advanced techniques to minimise scarring and discomfort, ensuring the best cosmetic outcome.
Prevention and Reducing Transmission
The HPV vaccine is the most effective way to prevent infection with high-risk HPV strains and those causing genital warts. In the UK, the vaccine is offered to children aged 12 to 13 as part of the routine immunisation programme. It protects against HPV types 16, 18, 6, and 11, which together account for most cervical cancers and genital warts.
The vaccine is also available privately for adults who were not vaccinated in school. Vaccination does not treat existing infections but prevents future ones.
Practicing safe sex reduces the risk of genital HPV transmission. Using condoms consistently lowers the chance of infection, though it does not eliminate it completely. Limiting the number of sexual partners also reduces exposure risk.
For non-genital warts, avoiding direct contact with warts and not sharing towels or razors can help prevent spread. Wearing flip-flops in communal showers and keeping your feet dry reduces the risk of verrucas.
If you have a wart, avoid touching or picking at it, as this can spread the virus to other parts of your body or to other people. Cover warts with a plaster when necessary, especially in shared spaces.
Regular cervical screening remains essential for women, even after vaccination. Screening detects cell changes early, allowing for monitoring or treatment before cancer develops.
When to Seek Specialist Care
You should consult a dermatologist or specialist if a wart is painful, bleeding, changing in appearance, or spreading rapidly. Warts on the face or genital area should always be assessed by a medical professional.
If you have multiple warts that are not responding to over-the-counter treatments, or if warts keep returning after treatment, a dermatologist can offer more effective options.
People with weakened immune systems, including those with diabetes or taking immunosuppressive medication, are more prone to persistent or severe HPV infections. These patients benefit from specialist review and tailored treatment.
Genital warts should always be evaluated by a doctor. They can resemble other conditions, and accurate diagnosis ensures you receive appropriate care.
At City Dermatology Clinic, our team includes some of the UK’s leading consultant dermatologists and plastic surgeons. We provide expert assessment and treatment for all types of warts and HPV-related skin conditions. No GP referral is needed, and same-day appointments are available at our central London location.
Frequently Asked Questions
Can HPV be cured?
There is no cure for the HPV virus itself. However, most infections clear naturally within two years as your immune system eliminates the virus. Treatments focus on removing visible symptoms such as warts rather than eradicating the virus.
Will warts come back after treatment?
Warts can recur, particularly if the virus remains active in your system. However, professional treatment significantly reduces recurrence rates compared to leaving warts untreated. Treating warts early and following aftercare advice improves long-term outcomes.
Are warts contagious?
Yes, warts are contagious and spread through direct contact with the wart or contaminated surfaces. Genital warts spread through sexual contact. Covering warts and avoiding touching them reduces transmission risk.
Is HPV the same as herpes?
No, HPV and herpes are different viruses. HPV causes warts and is associated with certain cancers. Herpes simplex virus causes cold sores and genital herpes, which appear as painful blisters. The two are unrelated and require different treatments.
Can I remove a wart at home?
Over-the-counter treatments can be effective for simple warts on the hands or feet. However, home removal carries risks of scarring, infection, or incomplete removal. Warts on the face, genitals, or those that are large or painful should be treated by a specialist.
How long does wart removal take?
Most wart removal procedures at City Dermatology Clinic take 15 to 30 minutes. Cryotherapy and electrosurgery are particularly quick. Healing time varies depending on the method used, but most patients recover within one to two weeks.
Do I need a GP referral to be seen?
No, you do not need a GP referral to visit City Dermatology Clinic. We offer direct access to consultant dermatologists and plastic surgeons, with same-day appointments available for urgent concerns.
Will wart removal leave a scar?
Our specialists use advanced techniques to minimise scarring. Small warts treated with cryotherapy or electrosurgery rarely leave noticeable scars. Larger warts removed surgically may leave a small scar, but this fades over time with proper aftercare.
HPV is common, but it is manageable with the right care. If you have concerns about warts or HPV-related skin conditions, our expert team at City Dermatology Clinic is here to help with same-day consultations and effective treatment options in central London.