A pyogenic granuloma is a benign overgrowth of small blood vessels that appears as a rapidly developing red or purple bump on the skin. Although not cancerous, it can bleed easily, grow quickly over a short period, and cause understandable concern. Because several other skin conditions can resemble a pyogenic granuloma, clinical assessment is important before treatment is considered.
At City Dermatology Clinic in London, lesions suspected to be pyogenic granulomas are assessed by experienced clinicians. Treatment decisions are based on examination, location, bleeding tendency, and individual patient factors. Removal is often straightforward, but technique and aftercare vary depending on the case.
What Is a Pyogenic Granuloma?
A pyogenic granuloma, also known as a lobular capillary haemangioma, is a benign vascular lesion. Despite the name:
- It is not caused by infection
- It does not contain pus
- It is not a true granuloma
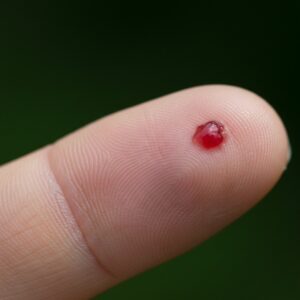
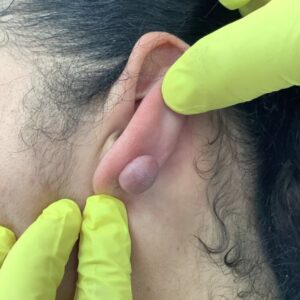
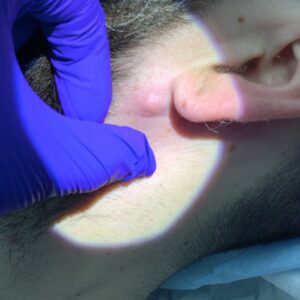
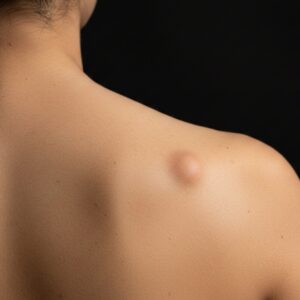
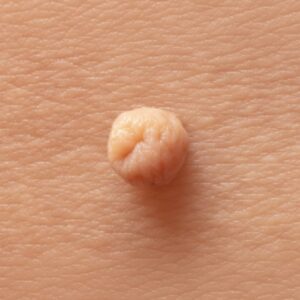
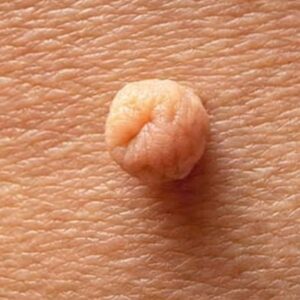
It typically appears as:
- A bright red, pink, or deep purple bump
- Smooth or slightly lobulated in surface
- Soft and prone to bleeding
- Rapidly growing over days to weeks
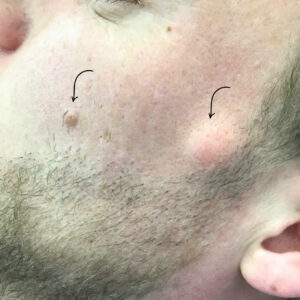
These lesions commonly develop on:
- Fingers and hands
- Face
- Lips
- Scalp
- Around the nail folds
They may follow minor trauma, although many patients do not recall a specific injury.
Why Do Pyogenic Granulomas Develop?
Pyogenic granulomas are thought to arise from an exaggerated healing response. When the skin experiences irritation or minor injury, new blood vessels form as part of normal repair. In some cases, this process becomes overactive, leading to a small vascular growth.
Factors associated with development include:
- Minor cuts or repetitive friction
- Ingrown nails
- Hormonal changes (particularly during pregnancy)
- Certain medications
- Previous surgical or dermatological procedures
In pregnancy, similar lesions may appear on the gums (often referred to as pregnancy epulis). Hormonal influence is believed to play a role in these cases.
Not all lesions have a clear trigger. Rapid growth is characteristic and often prompts patients to seek assessment.
When Should a Pyogenic Granuloma Be Assessed?
Although pyogenic granulomas are benign, other skin conditions can present in a similar way. Clinical review is advisable if a lesion:
- Has grown quickly
- Bleeds repeatedly or with minimal contact
- Appears ulcerated
- Changes in colour or surface texture
- Causes discomfort or interferes with daily activity
Certain skin cancers and vascular tumours can resemble a pyogenic granuloma, particularly when the lesion is atypical in appearance. For this reason, self-diagnosis is not recommended.
A consultation allows:
- Careful examination
- Consideration of alternative diagnoses
- Discussion of whether removal is appropriate
- Planning of treatment and histological analysis where indicated
Further chapters will cover diagnosis and treatment approaches in detail.
How Pyogenic Granulomas Are Diagnosed
Diagnosis is usually made through clinical examination.
During consultation at City Dermatology Clinic, the clinician will:
- Ask when the lesion first appeared
- Discuss how quickly it has grown
- Assess whether it bleeds easily
- Examine its size, shape, colour and base
- Consider any history of trauma or pregnancy
A dermatoscope (a magnified light device) may be used to examine vascular patterns more closely.
Although pyogenic granulomas have typical features, other conditions can appear similar. These include:
- Amelanotic melanoma
- Squamous cell carcinoma
- Basal cell carcinoma
- Other vascular lesions
If removal is performed, the tissue is usually sent for histological examination. Laboratory analysis confirms the diagnosis and excludes other pathology. Histology is particularly important when:
- The lesion is atypical
- The diagnosis is uncertain
- The growth pattern is unusual
- The patient has risk factors for skin cancer
Assessment is therefore not only about treatment planning, but also about diagnostic clarity.
Pyogenic Granuloma Treatment Options
Treatment is not always mandatory, but many patients choose removal because of bleeding, growth, or cosmetic concern.
The most appropriate technique depends on:
- Size of the lesion
- Depth and base involvement
- Anatomical location
- Patient age
- Risk of scarring
- Likelihood of recurrence
Surgical Excision
This is often the most definitive treatment.
- The lesion and its base are removed under local anaesthetic
- The wound is closed with sutures
- The specimen is sent for histology
Complete excision reduces the risk of recurrence because the deeper vascular component is removed.
Curettage and Cautery
This involves:
- Scraping the lesion away (curettage)
- Sealing the base using cautery to control bleeding
It may be suitable for smaller lesions. However, recurrence can occur if the base is not fully treated.
Shave Removal
A superficial shave technique may be considered in selected cases, particularly when the lesion is raised and well defined.
Suitability depends on lesion depth and location.
Laser or Cryotherapy
In certain cases, laser treatment or cryotherapy (freezing) may be considered. These are less commonly used for larger or deeply based lesions.
The choice of treatment is individual. During consultation, options are discussed in detail, including expected healing and potential scarring.
What to Expect During Removal
Most pyogenic granulomas can be removed in an outpatient setting.
The typical process includes:
- Cleaning the skin
- Injection of local anaesthetic (numbing the area)
- Removal of the lesion
- Control of bleeding
- Suturing if required
- Application of a dressing
Procedure time varies but is generally short.
Aftercare instructions are provided. These may include:
- Keeping the area clean and dry
- Avoiding excessive movement if sutures are present
- Returning for suture removal (if non-dissolvable sutures are used)
- Monitoring for signs of infection
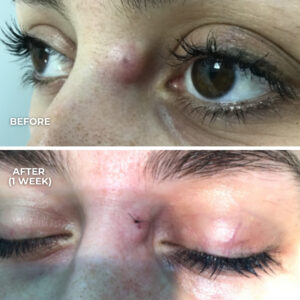
Healing time varies depending on lesion size and location. Areas with more tension or movement may take longer to settle.
If histology is performed, results are discussed once available.
Risks, Recurrence and Healing
Any procedure that removes a skin lesion carries potential risks. These are usually minor, but they are discussed during consultation before treatment proceeds.
Possible risks include:
- Bleeding (particularly as these lesions are vascular)
- Infection
- Delayed wound healing
- Scarring
- Recurrence of the lesion
Bleeding
Pyogenic granulomas contain many small blood vessels, which is why they bleed easily. During removal, bleeding is controlled using cautery or suturing. Mild oozing after the procedure can occur but usually settles with pressure.
Scarring
Any treatment that breaks the skin can leave a scar. The appearance depends on:
- Lesion size
- Location
- Skin type
- Individual healing response
- Technique used
Scars typically mature over several months and often become less noticeable with time. However, complete absence of scarring cannot be guaranteed.
Recurrence
Pyogenic granulomas can recur, particularly if the base is not fully removed. Recurrence does not suggest malignancy, but further treatment may be required.
Surgical excision generally has a lower recurrence rate compared with more superficial techniques, though no method eliminates risk entirely.
Healing time varies between individuals and between anatomical sites. Areas such as fingers or joints may take slightly longer due to movement.
Pyogenic Granulomas in Children
Pyogenic granulomas are relatively common in children and adolescents, particularly on the hands and face.
In children, reasons for seeking treatment often include:
- Repeated bleeding
- Accidental trauma during play
- Cosmetic concern
- Irritation or discomfort
Management depends on:
- Age of the child
- Size and location of the lesion
- Ability to tolerate local anaesthetic
- Parental preference following discussion
In some cases, treatment may be delayed if the lesion is small and not problematic. In others, removal may be appropriate to prevent ongoing bleeding.
Care is taken to minimise distress and to discuss realistic expectations regarding healing and scarring.
Pyogenic Granulomas During Pregnancy
Hormonal changes during pregnancy can increase the likelihood of developing vascular lesions, including pyogenic granulomas.
These may occur:
- On the hands
- On the face
- On the gums (often referred to as pregnancy epulis)
Some pregnancy-related lesions reduce in size after delivery. Others persist.
When a pyogenic granuloma develops during pregnancy, management is individualised. Considerations include:
- Severity of bleeding
- Rate of growth
- Gestational stage
- Patient preference
If the lesion is stable and not problematic, monitoring may be appropriate. If bleeding is frequent or significant, removal under local anaesthetic may be considered, provided it is clinically appropriate.
A consultation allows risks and timing to be discussed carefully within the context of pregnancy.