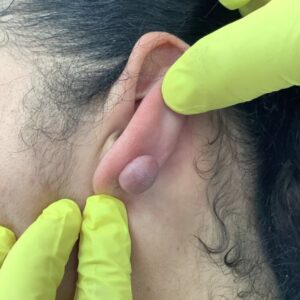
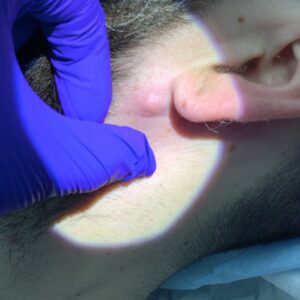
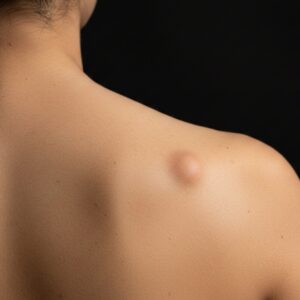
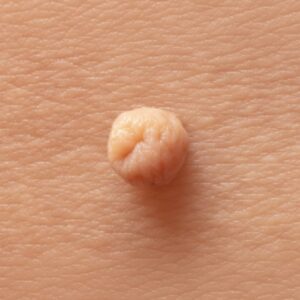
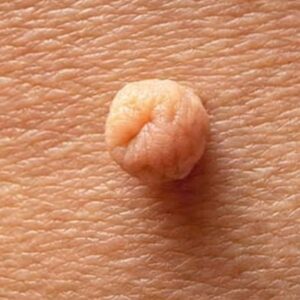
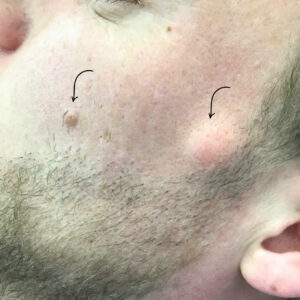
Skin tags are common, benign growths that often develop in areas where the skin rubs together, such as the neck, underarms, groin, or eyelids. They are usually painless and harmless. However, in some cases, a skin tag can become inflamed or infected, leading to noticeable changes that cause concern.
An infected skin tag may look red, swollen, or painful and can sometimes bleed or discharge fluid. These changes often prompt people to worry that something is wrong or that urgent treatment is needed. This article explains what an infected skin tag is, how it differs from simple irritation, and when medical assessment may be appropriate.
What is an infected skin tag?
An infected skin tag is a skin tag that has developed inflammation and bacterial involvement, usually following trauma or disruption to its surface. This can occur if the skin tag is repeatedly rubbed, twisted, scratched, or damaged, allowing bacteria to enter the skin.
It is important to distinguish infection from irritation, as the two can look similar but are managed differently. An irritated skin tag may appear red or sore for a short period, particularly after friction from clothing or jewellery. Infection, however, is more likely to cause ongoing pain, increasing redness, swelling, warmth, or discharge.
Skin tags that are narrow at the base can also twist on themselves, reducing blood supply. This may lead to sudden pain, darkening in colour, or inflammation, which can sometimes be mistaken for infection. A clinical assessment helps determine whether the changes are due to irritation, torsion, infection, or another skin condition that resembles a skin tag.
Because other lesions can occasionally be mistaken for skin tags, assessment is also important when symptoms are atypical or worsening.
Common symptoms that may suggest a skin tag is infected
An infected skin tag often looks and feels different from a typical, harmless skin tag. Symptoms usually develop after the area has been irritated or injured and tend to persist rather than settle within a day or two.
Common features may include:
- Redness spreading beyond the base of the skin tag
- Swelling or a feeling of tightness in the surrounding skin
- Pain or tenderness, especially when touched or rubbed
- Warmth in the area
- Discharge, which may be clear, yellow, or blood-stained
- Crusting or an unpleasant smell
In some cases, the skin tag may darken in colour or bleed more easily. These changes do not automatically indicate a serious problem, but they do suggest that the area is inflamed or infected rather than simply irritated.
Because symptoms can overlap with other skin conditions, ongoing or worsening changes are best assessed rather than monitored indefinitely at home.
Why skin tags can become infected
Skin tags are more likely to become infected when their surface is damaged. This often happens in areas of repeated friction, such as where clothing, skin folds, or jewellery rub against the lesion.
Common factors that increase the risk of infection include:
- Frequent rubbing or chafing
- Twisting or catching the skin tag accidentally
- Attempts to cut, tie off, or remove the skin tag at home
- Scratching or picking at the area
- Moist environments, which can encourage bacterial growth
Skin tags in areas such as the groin, underarms, or neck are particularly prone to these issues. Once the skin barrier is broken, bacteria that normally live on the skin can enter and cause infection.
Understanding why infection occurs helps explain why assessment is often recommended rather than repeated self-treatment, especially if symptoms are progressing rather than improving.
When an infected skin tag needs medical assessment
Not all inflamed skin tags require medical input, but assessment is advisable when symptoms suggest infection or are not settling on their own. In general, a clinician should assess the area if the skin tag:
- Becomes increasingly painful or swollen
- Shows spreading redness around the base
- Produces discharge or persistent bleeding
- Darkens in colour or changes suddenly in appearance
- Does not improve after a few days
- Is associated with fever or feeling generally unwell
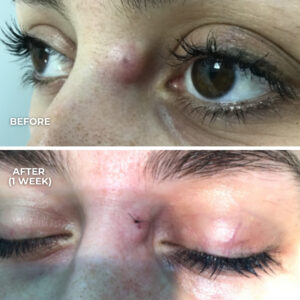
- Is located in a sensitive area such as the eyelid or genital region
Assessment is also appropriate if there is uncertainty about whether the lesion is truly a skin tag. Other skin growths can sometimes look similar but behave differently when inflamed or infected. A clinical examination helps clarify the cause and whether treatment or monitoring is most appropriate.
How infected skin tags are assessed and managed
During assessment, a clinician examines the skin tag and surrounding area to determine whether infection, irritation, torsion, or another condition is present. This includes looking at the size, colour, base of the lesion, and any discharge or surrounding skin changes.
Management depends on the findings. In some cases, the focus is on settling the infection or inflammation first rather than immediate removal. If removal is considered appropriate, the timing and method depend on factors such as the degree of infection, the location of the skin tag, and individual healing considerations.
Not all infected skin tags are suitable for same-day removal. A clinician may advise delaying removal until inflammation has settled, as this can reduce the risk of complications and support better healing.
Why self-treatment can make infection worse
Attempts to manage an infected skin tag at home can sometimes worsen the problem. Cutting, tying off, or applying home remedies can further damage the skin, increase inflammation, and introduce additional bacteria.
Self-treatment may lead to:
- Worsening infection
- Increased pain or bleeding
- Delayed healing
- Scarring or secondary skin problems
For this reason, ongoing symptoms are best assessed rather than repeatedly treated at home. Medical assessment helps ensure that the underlying issue is identified and managed appropriately, reducing the risk of further complications.